Hand hygiene is one of the most important elements of infection control. The aim of hand washing is to remove transient micro-organisms, acquired through everyday tasks in the clinical setting, from the surface of the hands. Good hand hygiene protects both patients and staff.
The WHO guidelines on “Hand Hygiene in Healthcare” describe five key situations where hand washing is required (the 5 moments for hand hygiene):
- Before touching a patient
- Before a clean or aseptic procedure
- After body fluid exposure risk
- After touching a patient
- After touching patient surroundings
There are two main cleansing agents used in hand washing; alcohol-based formulations and soap & water*. For both agents however, the technique used to clean the hands is the same.
To maintain optimum hand hygiene, it is recommended that nothing is worn below the elbows (except for a plain bands), and that the fingernails are clean and trimmed.
*The use of soap & water is specifically indicated when the hands are visibly soiled or when they have come into contact with spore-forming pathogens, such as clostridium difficile
Procedure
- Wet hands with water, and apply soap to cover hand surfaces
- Rub hands palm to palm
- Right palm over left dorsum with interlaced fingers and vice versa
- Palm to palm with fingers interlaced
- Backs of fingers to opposing palms with fingers interlaced
- Rotational rubbing of left thumb clasped in right palm and vice versa
- Rotational rubbing, backwards and forwards with clasped fingers of the right hand, and vice versa
- Rinse hands with water and dry with a single use towel
- Use the towel to turn off the tap
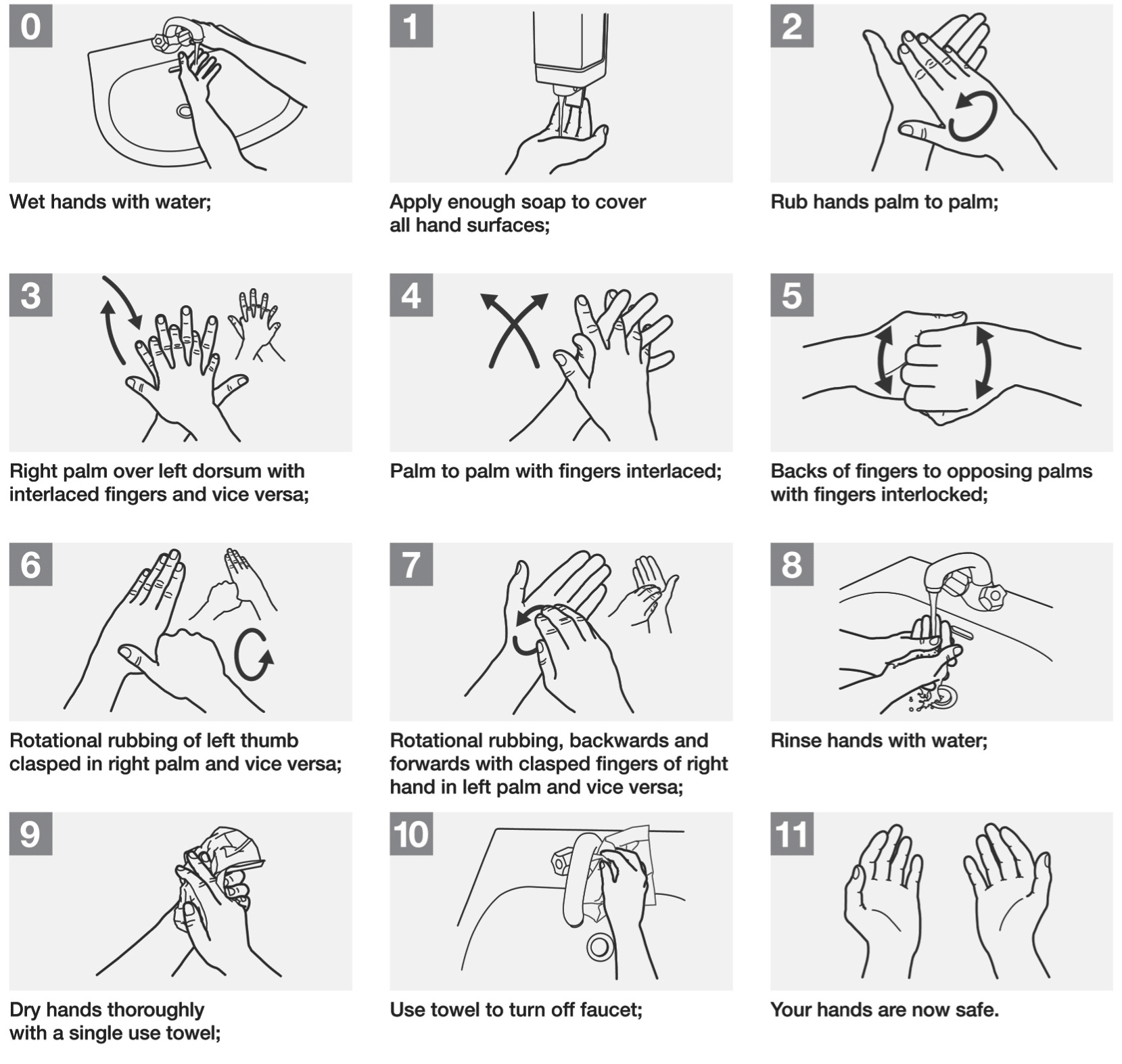
Figure 1 – Guide to handwashing, adapted from the WHO “How to Handwash” poster
Key Points
- Effective handwashing is an essential part in everyday clinical practice
- 5 key situations have been identified where handwashing is required
- Following the WHO ‘How to Handwash’ guidance will protect both patients and staff
