Introduction
Gynaecomastia is a condition by which males develop breast tissue due to an imbalanced ratio of oestrogen and androgen activity. It is usually a benign disease but breast cancer can develop in about 1% of cases.
It is a common condition with at least a third of men experiencing gynaecomastia in their lifetime and is usually an entirely reversible condition.
However, the condition often can cause embarrassment and can be of concern to the patient for a potential underlying malignancy.
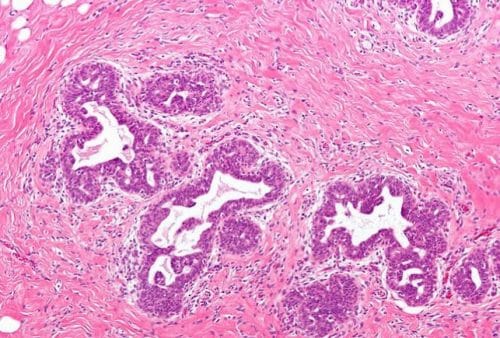
Figure 1 – Hyperplasia of the breast tissue, as seen in as a case of gynaecomastia
Pathophysiology
Physiological gynaecomastia most commonly occurs in adolescence, resulting from the delayed testosterone surge relative to oestrogen at puberty. Less commonly it occurs in the older population, secondary to decreasing testosterone levels with increasing age.
Pathological gynaecomastia results from changes in the oestrogen:androgen activity ratio and there are a variety of underlying mechanisms:
- Lack of testosterone
- Causes include Klinefelter’s syndrome, androgen insensitivity, testicular atrophy, or renal disease
- Increased oestrogen levels
- Causes include liver disease, hyperthyroidism, obesity, adrenal tumours, or certain testicular tumours (e.g. Leydig’s cell tumours)
- Medication*
- Common causative agents include digoxin, metronidazole, spironolactone, chemotherapy, goserelin, antipsychotics, or anabolic steroids
- Idiopathic
*25% of all cases, either through an increased oestrogen activity or reduced testosterone activity
Clinical Features
Gynaecomastia often has an insidious onset. Ensure to ask about associated symptoms and co-morbidities during assessment, and to assess for clinical features of potential underlying causes, including malignancy, during examination*
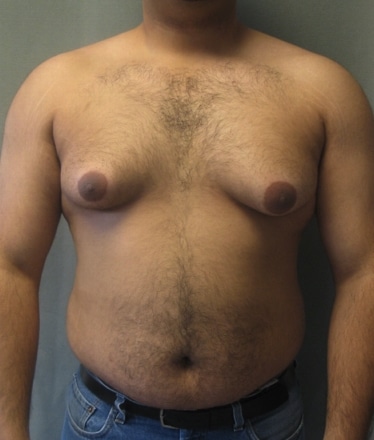
On examination, gynaecomastia will present as a rubbery or firm mass (typically >2cm diameter) that starts from underneath the nipple and spreads outwards over the breast region (Fig. 2).
Ensure to assess for any evidence of breast malignancy.
*A testicular examination is essential, especially in young patient presenting with the condition
Differential Diagnosis
The main differential is pseudogynaecomastia, adipose tissue in the breast region associated with being overweight*.
*This can usually be tested on examination by pinching to see if there is an obvious disc of breast tissue present however if not palpable then further imaging and / or histology may be required to definitively exclude
Investigations
Tests are only necessary if the cause for gynaecomastia is unknown (especially if physiological or iatrogenic). In cases where malignancy is suspected, patients will require the triple assessment.
In cases where the causes in unknown, liver and renal function (U&Es and LFTs) should be checked initially, before checking the hormone profile if these are normal; the levels of lutenising hormone (LH) and testosterone can indicate different clinical pictures:
- LH high and testosterone low = testicular failure
- LH low and testosterone low = increased oestrogen
- LH high and testosterone high = androgen resistance or gonadotrophin-secreting malignancy
Management
The management ultimately depends on the causative factors and the phase of gynaecomastia. If there is a reversible underlying cause, then treatment or reversal of this should also allow for the resolution of the gynaecomastia as well.
In most cases, reassurance may be enough for the patient; Tamoxifen can also be used in cases to help alleviate symptoms, especially tenderness. In patients with later stages of fibrosis, surgery may be the only option if medical treatments have failed.
Key Points
- Pathological gynaecomastia occurs from changes in the oestrogen:androgen activity ratio
- It will present as a rubbery or firm mass, starting from underneath the nipple and spreading outwards over the breast region
- Tests are only necessary if the cause for gynaecomastia is uncertain; any suspicion of malignancy requires the triple assessment