Introduction
Rectal bleeding (or haematochezia) is the passage of fresh blood per rectum. It is generally caused by bleeding from the lower gastrointestinal tract, but may occur in patients with large upper GI bleeds or from small bowel lesions.
The causes of rectal bleeding range from benign to life-threatening disease and can result in significant haemodynamic instability if not managed appropriately.
In this article, we shall look at the causes, key clinical features, investigations, and management of haematochezia.
Differential Diagnosis
Fresh rectal bleeding most commonly results from a source in the rectum or colon, however large upper GI bleeds can also present with haematochezia*
Common causes of acute lower GI bleeding include diverticular disease, ischaemic or infective colitis, haemorrhoids, malignancy, angiodysplasia, Crohn’s disease or Ulcerative colitis, or radiation proctitis.
Diverticulosis
Diverticulosis is the most common cause of lower gastrointestinal bleeding. Diverticula are outpouchings of the bowel wall that are composed only of mucosa, most commonly in the descending and sigmoid colon.
The incidence of diverticulosis increases with age. Whilst diverticular disease bleeds are often painless, any bleeds secondary to diverticulitis can often be painful, due to the localised inflammation.
Haemorrhoids
Haemorrhoids are pathologically engorged vascular cushions in the anal canal that can present as a mass, with pruritus, or fresh red rectal bleeding.
The blood is classically on the surface of the stool or toilet pan, rather than mixed in with it. Large haemorrhoids can also thrombose, which can be extremely painful.
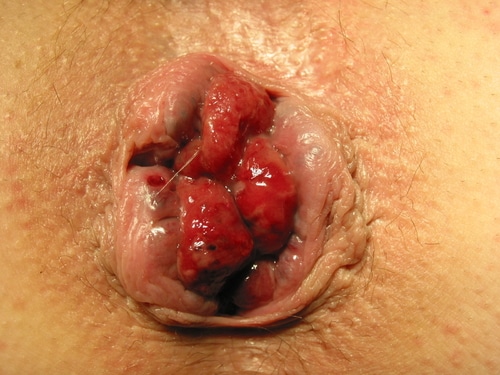
Figure 2 – Haemorrhoids located in the 3, 7, and 11 o’clock positions
Malignancy
With any case of PR bleeding, especially in the elderly population, malignancy should be suspected, as this may be a colorectal cancer.
In the assessment of any patient with haematochezia, it is important to enquire about other lower GI symptoms, weight loss, or relevant family history, potentially suggestive of a malignancy.
Clinical Features
Key aspects of the clinical history to ascertain from a patient presenting with PR bleeding include:
- Nature of bleeding – duration, frequency, and colour of the bleeding, and whether related to stool and defecation
- Associated symptoms – including pain (especially association with defaecation), any haematemesis or melena, any PR mucus, previous episodes, or weight loss
- Family history – bowel cancer or inflammatory bowel disease
Examine the abdomen for any localised tenderness or palpable masses. A PR examination is essential for every patient presenting with haemotochezia, allowing assessment for any rectal masses and ongoing presence of blood.
All haemodynamically unstable bleeds should be approached in an A to E manner, and have a different approach than to stable bleeds.
The Oakland Score
The Oakland Score can be used to help stratify patients presenting with a lower GI bleed to determine if outpatient management is feasible.
Factors used to determine the Oakland score are Age, Sex, Previous Admissions for Lower GI bleeding, PR findings, Heart Rate, Systolic Blood Pressure, and Haemoglobin Concentration.
Investigations
All patients presenting with rectal bleeding should have routine bloods* (FBC, U&Es, LFT, clotting) and a Group and Save requested (as a minimum). Stool cultures are also useful to exclude infective causes.
In patients who are haemodynamically unstable, patients should be initially resuscitated using blood products and any coagulopathy corrected. An urgent CT angiogram (before any endoscopic therapy) should be performed once stabilised (even if partially). This can identify the source of bleeding, as well as permitting potential therapeutic intervention with embolisation.
*Acute bleeds may not initially show reduced Hb level due to haemoconcentration, however ongoing bleeding will show a reduced Hb; the presence of an elevated serum urea to creatinine ratio suggests an upper GI source of bleeding being more likely
Further Investigations
Patients with stable bleeds will require a colonoscopy for further assessment, importantly to exclude left-colonic pathology (especially malignancy); this can often be performed as an outpatient if the patient remains well.
In stable patients with PR bleeding and no abnormality identified on colonoscopy, upper GI endoscopy (OGD) should subsequently be performed to look for any upper GI causes for bleeding.
If this proves inconclusive, further investigations such as capsule endoscopy or RBC scintigraphy may be required.
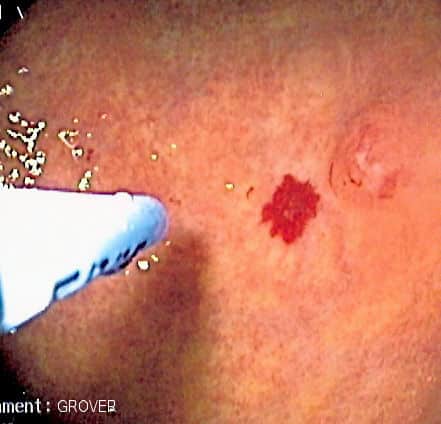
Figure 3 – Endoscopic image of angiodysplasia being treated with argon plasma coagulation
Key risk factors for adverse outcomes from any acute rectal bleeding include haemodynamic instability, ongoing haematochezia, age >60yrs , serum creatinine >150µmol/L, or the presence of significant co-morbidities.
Management
95% of cases will settle spontaneously. Often young haemodynamically stable patients, in who the bleeding has stopped and have a low risk score, can be discharged and investigated as an outpatient.
Any unstable rectal bleeding warrants urgent resuscitation, with a standard A to E approach; wide bore intravenous access should be obtained and blood products given until the patient stabilises.
Any patient with a Hb <70g/L (or Hb <80g/L in those with cardiovascular disease) should will typically also require a blood transfusion. Patients on anti-coagulation should have this reversed urgently, with guidance from a haematologist as required.
Potential further management options include:
- Endoscopic haemostasis methods include injection (typically diluted adrenaline), contact and non-contact thermal devices (such as bipolar electrocoagulation or argon plasma coagulation), and mechanical therapies (endoscopic clips and band ligation)
- Arterial embolisation is possible in those with an identified bleeding point (termed a “blush”) of sufficient size on angiogram
Surgical Intervention
Surgical intervention is rarely required, however may be considered in patients with ongoing lower GI bleeding with instability (or requiring continued transfusion), where endoscopic and radiographic treatment has failed.
Key Points
- Any patient with rectal bleeding required a flexible sigmoidoscopy or colonoscopy
- A patient with a large fresh rectal bleed who is haemodynamically unstable has an upper GI bleed until proven otherwise
- Acute bleeds may not initially show an anaemia in the full blood count
- Patients who are haemodynamically unstable need an emergency OGD and colonoscopy