Introduction
A surgical site infection (SSI) is an infection that occurs in the incision created by an invasive surgical procedure.
SSI is a leading cause of hospital morbidity, resulting in prolonged hospital stay, increased hospital costs, higher rates of re-operation, and even increased mortality rates. Primary management is prevention through good surgical technique and patient optimisation.
The rates of SSI vary depending on the type of surgery, increasing with worsening level of contamination. SSIs can be classified based on the tissues involved:
- Superficial SSI = limited to skin and subcutaneous tissue
- Deep SSI = affecting the fascial and muscular layers
- Cavity space infection = within an abdominal or joint cavity
In this article, we shall look at the risk factors, clinical features, and management of surgical site infections.
Risk Factors
There are several factors that increase the risk of a surgical site infection, as shown in Table 1:
| Patient Factors | Operation Factors |
|
|
Table 1 – Risk Factors for Surgical Site Infections
Clinical Features
The symptoms of a surgical site infection typically appear 5 to 7 days post-procedure, however can develop up to 3 weeks after (especially if a prosthesis is inserted).
The common clinical features of surgical site infections include:
- Spreading erythema
- Localised pain
- Pus or discharge from the wound
- Persistent pyrexia
In certain cases, superficial or even complete wound dehiscence (FIg. 1B) can occur secondary to SSI developing. Most SSIs are superficial, however some can result in extensive wound breakdown; fortunately, the need for debridement is not common.
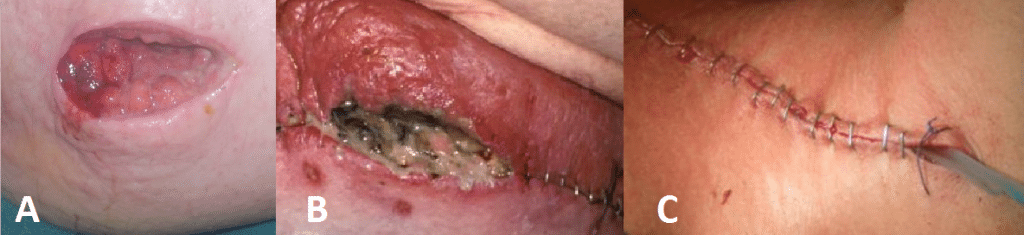
Figure 1 – (A) Purulent discharging forming in open wound; (B) Erythema and pus seen in closed wound; (C) drain placed in situ intra-operatively
Investigations
Any surgical site infection should have wound swabs taken for culture at the wound site, especially if a purulent discharge is present (avoiding wound edges where possible to reduce skin flora contamination).
Blood tests for infection markers (FBC, CRP) should be taken, alongside blood cultures if any evidence of systemic involvement or sepsis.
If the clinical picture (e.g. septic patient with very raised inflammatory markers) does not match the appearances of the wound, consider cross-section imaging to assess for deeper collections or even necrotising fasciitis.
Management
Any sutures or clips present should be removed, allowing for the drainage of any pus and the opportunity for wound packing if required.
Empirical antibiotic should be started; different wounds are often caused by different organisms (e.g. a laparotomy wound infection is more likely to be caused by a coliform), therefore best practice is to follow local empirical antibiotic guidelines. Antibiotic therapy can then be tailored following culture results.
Most patients with an SSI will response well with the above management steps
Prevention
The prevention of surgical site infections can be achieved in the pre-operative, intra-operative, and post-operative settings.
Pre-Operative Phase
- Give prophylactic antibiotics if indicated (clean surgery involving a prosthesis, clean-contaminated surgery, or contaminated surgery)
- Do not remove hair routinely – if necessary do this immediately prior to surgery with an electric clipper
- Patient advice – encourage weight loss and smoking cessation, optimise nutrition (to promote wound healing) and ensure good diabetic control if applicable
Intraoperative Phase
- Prepare the skin at the surgical site immediately before the incision using an antiseptic preparation
- Chlorhexidine has been shown to be more effective than Betadine for skin preparation
- Change gloves or gowns if contaminated
- Wound irrigation at closure and use of antibiotic-impregnated sutures to close
Post-Operative Phase
- Monitor wounds closely, especially those in difficult areas, such as skin creases and underneath skin folds (such as groin), are closely observed
- Refer to a tissue viability nurse for advice on appropriate dressings for the management of surgical wounds that are healing by secondary intention
Key Points
- Surgical site infections are a leading cause of in hospital morbidity, rates dependent on the type of surgery performed
- Often appearing 5-7 days post-operatively, symptoms include spreading erythema, localised pain, pus/discharge from the wound, or a persistent pyrexia
- Primary prevention is the optimal way in reducing surgical site infections, with several evidence-based interventions possible
- Any case of surgical site infection should be regularly monitored, with any clips or sutures removed where feasible, any pus present is suitably drained, and empirical antibiotics prescribed
