Introdcution
Urinary tract infection (UTI) is a common post-operative complication for various surgical procedures.
Patients that develop UTIs in the peri-operative period have higher rates of mortality and longer length of stay, so it is important that they are promptly recognised and managed.
Common causative organisms are E. coli, Klebsiella sp., Enterobacteur sp., Proteus sp., Pseudomonas sp., and Staphylococcus sp.
Risk Factors
There are several factors that increase the risk of developing post-operative urinary tract infection:
- Age > 60yrs
- Female
- Significant co-morbidities (e.g. renal failure, diabetes mellitus)
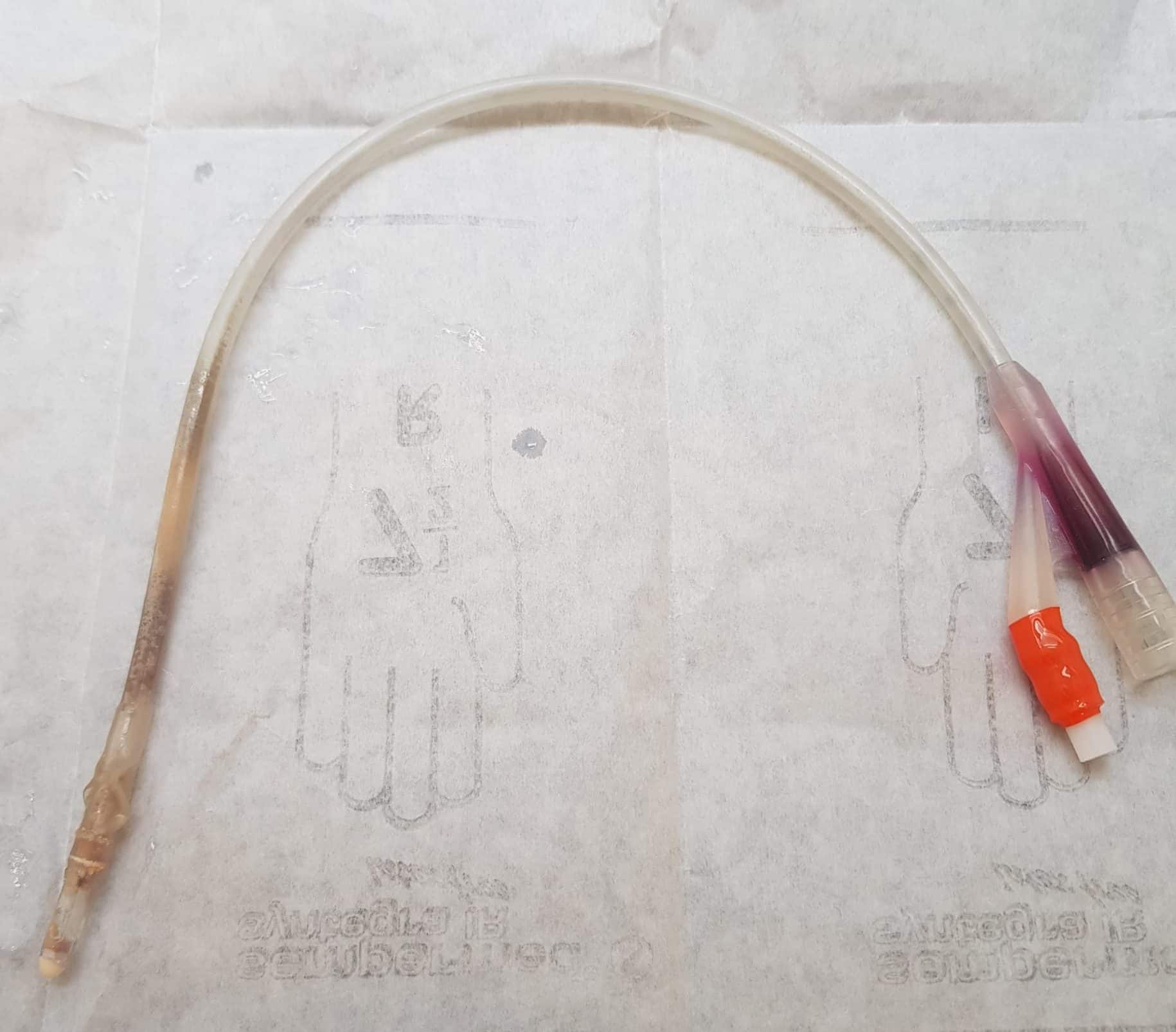
- Catheterisation (Fig. 1) or recent instrumentation
- Pregnancy
- Urinary retention or renal stones
Clinical Features
The classical clinical features of UTI are urinary frequency, urgency, and dysuria. On examination, these patients may have mild suprapubic pain and be pyrexial.
A UTI should also be considered in the any patient who presents:
- With delirium
- Septic (without a clear foci of infection)
- In acute urinary retention
It is also important to assess for features of pyelonephritis as well (such as loin pain, renal angle tenderness, or pyrexia).
Investigations
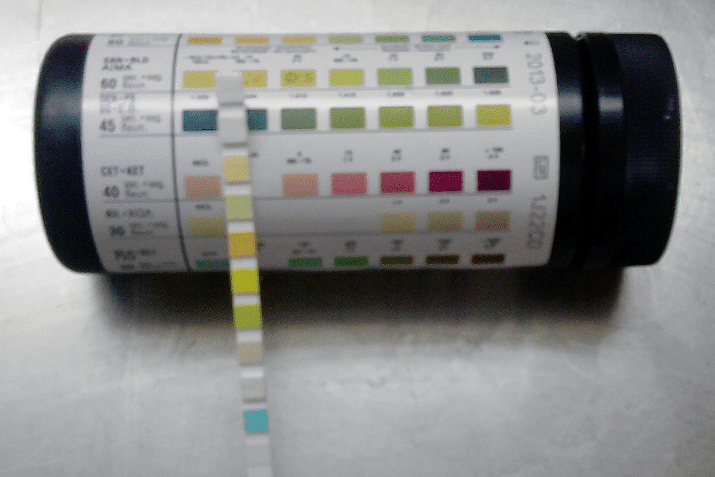
A urine dipstick* should be performed initially for all suspected cases (even despite a high rate of contamination seen in the elderly population).
*Sterile pyuria is the presence of an elevated white cell count in the urine however no organisms are identified using standard culture techniques; causes of sterile pyuria include an inadequately-treated UTI, a sexually-transmitted infection, or renal stones

Figure 1 – Urine should be inspected for turbidity and urine dipstick performed
If the urine dipstick is positive (nitrites* or leukocyte esterase ± blood) or clinical features in keeping with UTI, then a sample of the urine should be sent off for microscopy, culture, and sensitivities (MC&S). These are usually referred to as a “mid-stream urine (MSU)” or, if the patient is catheterised, a “catheter specimen of urine (CSU)’”.
Depending on the clinical picture, routine blood tests may be considered, including FBC, CRP, and U&Es. In those who are systemically unwell, blood cultures (for any septic patient) and a venous blood gas (VBG, to assess for tissue perfusion with the lactate) may be warranted.
A bladder scan may be required if the patient has potentially entered retention; if this is the case, catheterisation is typically indicated. If pyelonephritis is suspected or in cases of recurrent UTIs, a renal US or further definitive imaging may be required to check for obstructive causes.
*Most Gram-negative bacteria will convert nitrates to nitrites, so can be used as a surrogate marker for a urinary infection
Management
Ensure the patient is well hydrated (either through PO or IV routes) and maintains a satisfactory urine output (>0.5mL/kg/hour)
Definitive management is via antibiotic therapy, referring to your local antimicrobial guidelines; classically trimethoprim, nitrofurantoin, or co-amoxiclav are typical antibiotic choices.
The majority of UTIs will resolve from the empirical treatment, yet adapt accordingly following MC&S results if poor response. Any catheterised patients with a UTI should have their catheter changed prior to starting any antibiotics.
Key Points
- The classical features of a UTI are urinary frequency, urgency, dysuria, and pyrexia
- Urine dipstick +/- MCS will aid the diagnosis of a UTI
- Start empirical antibiotic therapy and ensure adequate hydration
- Change any long-term urethral or suprapubic catheter in-situ in the presence of a UTI