Introduction
Deep Venous Insufficiency (DVI) is a chronic disease that can result in significant morbidity. It is commonly caused either by deep vein thrombosis (DVT) or valvular insufficiency, and together with varicose veins (in the superficial venous system) it is part of chronic venous insufficiency.
Deep Venous Insufficiency occurs as a result of a failure of the venous system, characterised by valvular reflux, venous hypertension and obstruction*.
Prevalence of DVI is around 10-15% and is more common in women. Causes can be divided into:
- Primary, whereby there is an underlying defect to the vein wall or valvular component
- Includes congenital defects and connective tissue disorders
- Secondary, whereby defects occur secondary to damage
- including post-thrombotic disease, post-phlebitic disease, venous outflow obstruction, and trauma
*The pathophysiology is similar to that of varicose veins but it affects the deep venous system, instead of superficial veins
Risk Factors
Risk factors for DVI include increasing age, female gender, pregnancy, previous DVT or phlebitis, obesity, and smoking.
Those in jobs which involve long periods of standing or with a strong family history of venous disease are also at risk.
Clinical Features
Patients may report chronically swollen lower limbs, which can become aching, pruritic, and painful. They may also report venous claudication, characterised by a bursting pain and tightness on walking which resolves on leg elevation.
On examination, several signs can indicate underlying DVI, including varicose eczema (dry and scaly skin), thrombophlebitis, haemosiderin skin staining, lipodermatosclerosis*, or atrophie blanche**
Patients will have varying degrees of dependent pedal oedema and may also have venous ulcers, which are typically found over the medial malleolus
*A tapering of legs above ankles, an “inverted champagne bottle” appearance **Localised round, white atrophic regions surrounded by dilated capillaries
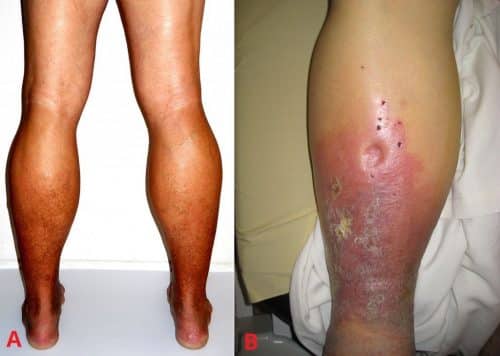
Figure 1 – (A) Haemosiderin deposition with lipodermatosclerosis (B) Pitting oedema with varicose eczema
Patients who have had a prior DVT may present with symptoms of Post-Thrombotic Syndrome*, including heaviness, cramps, pain, pruritis, and paraesthesia, and clinical signs of pretibial oedema, skin induration, hyperpigmentation, venous ectasia, redness, and ulceration.
*The Villalta scale can be used to assess progression with treatment of post-thrombotic syndrome
Differential Diagnosis
Differential diagnoses to consider in patients who present with leg swelling include renal, hepatic, or cardiac disease, all of which require thorough work-up and investigation before being excluded. Any ulceration will need careful evaluation of the underlying cause.
Investigations
The primary investigation for diagnosing DVI is a Doppler ultrasound scan, allowing the assessment for the extent of venous reflux*, any sites of stenosis, and the presence of a DVT or varicose veins.
Routine blood tests may be useful to further exclude other potential aetiologies, including FBC, U&Es, and LFTs, BNP (+/- an ECHO if indicated).
An essential component of the investigations is documentation of foot pulses and ankle brachial pressure index as this will be required to determine suitability for compression therapy.
*If there is evidence of a venous occlusion or reflux in the pelvis as characterised by poor flow wave forms in the femoral veins or varicosities over the buttocks/perineum, then an MR Venogram may be performed
Management
Identifying deep venous insufficiency early is essential, as early treatment may reduce long-term complications and prevent irreversible damage. Management can be either conservative or surgical.
The mainstay of conservative treatment is via compression stockings (Fig. 2). If the patient has a venous ulcer then they should be started in full compression treatment, such as with 4-layer bandage, short stretch bandage, stockings, or compression wrap. Patients without ulceration can be started in light compression stockings (Class 1) and build up (to Class 4) as required, depending on symptoms.
If symptoms remain, elevating the feet above the level of the precordium can reduce symptoms and disease progression.

Figure 2 – Compression stockings, both below knee and above knee
Surgical Management
Surgical management of deep venous insufficiency is variable. There is minimal evidence in the benefit for valvuloplasty and this is not routinely undertaken.
Patients with severe post-thrombotic syndrome with an occluded iliac vein may be suitable for deep venous stenting; this procedure is reserved for patients with the most severe symptoms* despite maximal conservative therapy, and requires veins with a good inflow and outflow at the site around where the stent is placed.
*When undertaken in the right patient, stent patency is over 80% out to 3 years, with significant improvements in quality of life
Complications
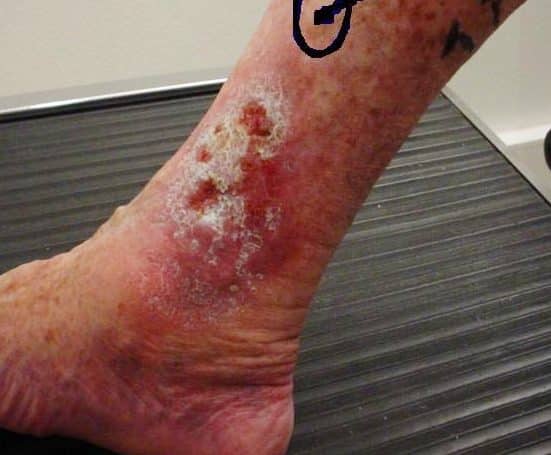
Common long-term complications of DVI include swelling, recurrent cellulitis, chronic pain and ulceration (Fig. 3). More serious but less common complications include deep vein thrombosis, secondary lymphoedema, and varicose veins.
A Marjolin ulcer is a rare type of cutaneous squamous cell carcinoma (SCC) developing at the site of severe or recurrent inflammation (such as in venous insufficiency). They typically present as non-healing ulcers, steadily increasing in size and have excessive granulation tissue, often bleeding easily on contact, and be painful.
Key Points
- Deep Venous Insufficiency is a common condition yet requires careful work-up for a diagnosis to be made
- Gold standard investigation is via a Doppler US scan, which can also aid to exclude DVT
- Management is primarily conservative, but surgical treatment is an option
- Complications include ulcer formation, recurrent cellulitis, chronic pain, and DVT